Supplements for Neuropathy in Feet: What Actually Works
The burning, tingling, and numbness in your feet from neuropathy can make every step feel like walking on hot coals. If you’re searching for supplements that actually help, the good news is that a handful of ingredients have real clinical evidence behind them. Alpha-lipoic acid, B vitamins, and acetyl-L-carnitine top the list, with published trials showing measurable improvements in nerve pain and function. Below, I’ll walk you through seven supplements backed by research, the dosages used in clinical studies, and the safety warnings you need to know before trying any of them.
Medical Disclaimer: This article is for educational purposes only and is not medical advice. Neuropathy can result from diabetes, autoimmune conditions, infections, medications, and other causes. Always consult your physician before starting any supplement, especially if you take prescription medications or have kidney or liver disease.
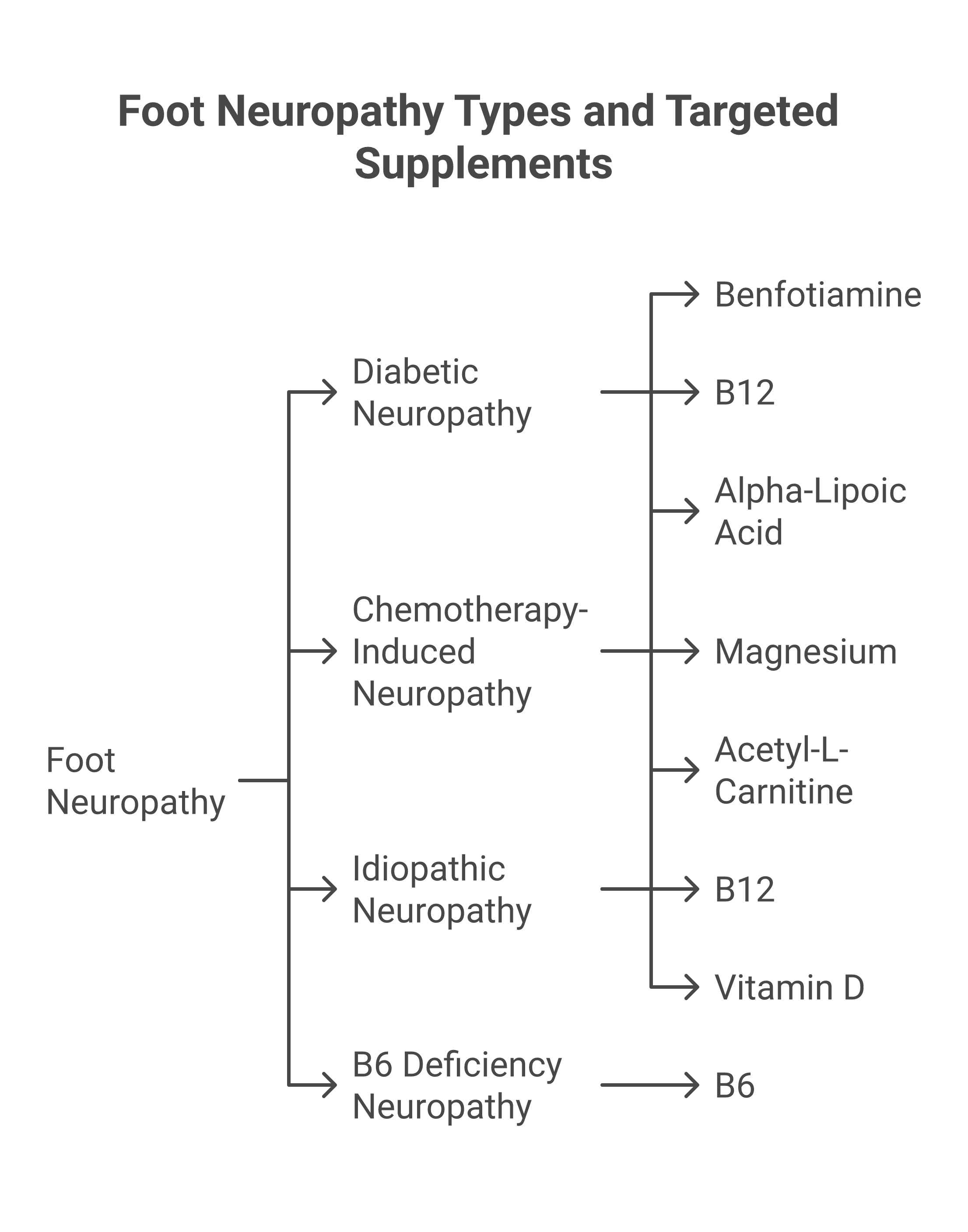
Why Foot Neuropathy Is So Common (and So Hard to Treat)
Peripheral neuropathy affects an estimated 20 million Americans, according to the National Institute of Neurological Disorders and Stroke. The feet are almost always the first place symptoms show up. That’s because the longest nerves in your body run from your spinal cord all the way down to your toes, and those distant nerve endings are the most vulnerable to damage.
Diabetic neuropathy is the single most common cause. Roughly 50% of people with diabetes will develop some form of neuropathy during their lifetime, according to the American Diabetes Association. High blood sugar damages small blood vessels that feed your nerves, starving them of oxygen and nutrients. But diabetes isn’t the only culprit. Chemotherapy drugs, alcohol use, vitamin deficiencies, autoimmune conditions, and sometimes no identifiable cause (called idiopathic neuropathy) can all trigger the same burning, tingling, and loss of sensation in the feet.
Standard medical treatments include gabapentin, pregabalin, duloxetine, and topical capsaicin. These can help manage pain, but they don’t address the underlying nerve damage. That’s where targeted supplementation may fill a gap, especially for people whose neuropathy involves nutritional deficiencies or oxidative stress.
If you’re also dealing with joint stiffness alongside nerve pain, our guide to joint supplements for seniors covers ingredients that may help with mobility.

1. Alpha-Lipoic Acid (ALA): The Strongest Evidence for Foot Neuropathy
Alpha-lipoic acid has more clinical trial data behind it than any other supplement for peripheral neuropathy. It’s a naturally occurring antioxidant that your body produces in small amounts, and it works in both water and fat, giving it access to nerve cells that other antioxidants can’t reach.
The landmark ALADIN trial (published in Diabetologia, 1995) tested intravenous ALA at 600 mg daily for three weeks. The group receiving 600 mg saw their Total Symptom Score (a composite measure of pain, burning, tingling, and numbness in the feet) drop by 63.5% from baseline, with a response rate of 82.5%. A later meta-analysis published in the International Journal of Endocrinology (Mijnhout et al., 2012) confirmed that 600 mg/day of ALA, whether given intravenously or orally, produced significant reductions in neuropathic symptoms compared to placebo.
The oral dosing evidence is especially relevant if you’re supplementing at home. The SYDNEY 2 trial showed that oral ALA at 600 mg once daily for five weeks significantly reduced stabbing pain, burning, and numbness in the feet. Higher doses (1,200 mg and 1,800 mg) didn’t produce meaningfully better results but did increase gastrointestinal side effects like nausea.
Dosage used in studies: 600 mg/day orally, taken on an empty stomach 30 minutes before meals. This is the dose with the best balance of effectiveness and tolerability.
Safety notes: ALA can lower blood sugar, so people with diabetes should monitor their glucose carefully and talk to their doctor about potential medication adjustments. Mild GI upset is the most common side effect.
2. Vitamin B12 (Methylcobalamin): Essential for Nerve Myelin
Vitamin B12 deficiency is one of the reversible causes of peripheral neuropathy, and it’s surprisingly common in older adults. Your body needs B12 to produce myelin, the protective sheath that wraps around nerve fibers. Without enough myelin, nerve signals slow down or misfire, producing the classic tingling and numbness in the feet and hands.
A 2021 randomized, double-blind, placebo-controlled trial published in Nutrients (Didangelos et al.) studied 90 patients with type 2 diabetes and neuropathy. Those who received 1,000 mcg of oral methylcobalamin daily for one year showed significant improvements in nerve conduction velocity, sudomotor function (sweat gland nerve testing), pain scores, and quality of life compared to the placebo group.
Why methylcobalamin over cyanocobalamin? Methylcobalamin is the active form your nervous system uses directly. Cyanocobalamin (the cheaper form found in many supplements) requires your body to convert it first, and that conversion becomes less efficient with age. People over 60 are at particular risk for B12 deficiency because stomach acid production declines, reducing B12 absorption from food.
Metformin, a common diabetes medication, also depletes B12 over time. A study published in the Journal of Clinical Endocrinology and Metabolism found that long-term metformin use was associated with a 13% reduction in B12 levels.
Dosage used in studies: 1,000 mcg (1 mg) of methylcobalamin daily, orally. In cases of severe deficiency or malabsorption (Crohn’s disease, gastric bypass, pernicious anemia), injections of 1,000-1,500 mcg may be more effective.
Safety notes: B12 is water-soluble with no established upper limit for toxicity. Excess amounts are excreted in urine. However, get your B12 levels tested before supplementing, as high-dose B12 can mask a folate deficiency.
For a broader look at nerve support ingredients, see our guide to the best nerve support supplements for seniors.
3. Benfotiamine (Fat-Soluble Vitamin B1): Blocks Nerve-Damaging Pathways
Benfotiamine is a fat-soluble form of vitamin B1 (thiamine) that crosses cell membranes more easily than regular thiamine. This matters because it can reach nerve tissue at higher concentrations. Regular thiamine is water-soluble and poorly absorbed at high doses.
The BENDIP trial (Stracke et al., published in Experimental and Clinical Endocrinology and Diabetes, 2008) randomized 165 patients with diabetic polyneuropathy to receive benfotiamine at 600 mg/day, 300 mg/day, or placebo for six weeks. The 600 mg group (300 mg twice daily) showed a statistically significant improvement in the Neuropathy Symptom Score compared to placebo. The 300 mg/day group did not reach statistical significance.
An earlier pilot study (BEDIP trial, Haupt et al., 2005) also found significant improvement in neuropathy scores at 400 mg/day over three weeks. Benfotiamine works by blocking advanced glycation end-products (AGEs), which are toxic compounds formed when blood sugar is chronically elevated. AGEs directly damage nerve cells and blood vessels.
Dosage used in studies: 300 mg twice daily (600 mg total) for at least six weeks. The 600 mg dose showed significant results where 300 mg did not.
Safety notes: Benfotiamine is generally well tolerated with few reported side effects. Because it specifically targets glucose-driven nerve damage, it is most relevant for diabetic neuropathy rather than other neuropathy types.
4. Acetyl-L-Carnitine (ALC): Supports Nerve Fiber Regeneration
Acetyl-L-carnitine is an amino acid derivative that supports mitochondrial energy production in nerve cells. Unlike most supplements on this list, ALC has shown evidence of actually promoting nerve fiber regeneration, not just reducing symptoms.
A pooled analysis of two randomized, placebo-controlled trials published in Diabetes Care (Sima et al., 2005) studied 1,257 patients with diabetic neuropathy. Patients received ALC at either 500 mg or 1,000 mg three times daily for one year. The 3,000 mg/day group showed significant improvements in pain, nerve regeneration (measured by sural nerve biopsy), and vibratory perception at both 26 and 52 weeks. The 1,500 mg/day group showed improvement in pain but not in the nerve regeneration measures.
A systematic review and meta-analysis in PLOS ONE (Li et al., 2015) confirmed that ALC produced a significant 20.2% pain reduction compared to placebo across multiple trials, with benefits appearing more consistent at doses above 1,500 mg/day.
Dosage used in studies: 1,000 mg three times daily (3,000 mg/day total) for the strongest evidence of nerve regeneration. Lower doses of 1,500-2,000 mg/day may still help with pain reduction.
Safety notes: ALC can cause mild nausea, stomach upset, and restlessness. It may interact with blood thinners (warfarin) and thyroid medications. People with seizure disorders should use caution, as ALC may lower seizure threshold in some individuals.
5. Vitamin D: The Deficiency That Makes Neuropathy Worse
Vitamin D isn’t a direct nerve repair supplement, but deficiency is strongly associated with worse neuropathy outcomes, especially in people with diabetes. A 2024 study in Frontiers in Endocrinology found that vitamin D deficiency was independently associated with subclinical diabetic peripheral neuropathy across all age groups: youth (OR 2.43), middle-aged adults (OR 1.96), and elderly patients (OR 1.44).
The mechanism involves both nerve protection and inflammation control. Vitamin D receptors exist on nerve cells, and the vitamin helps regulate inflammatory cytokines that can damage peripheral nerves. A study published in Frontiers in Nutrition (2021) found that patients with severe vitamin D deficiency (below 16 ng/mL) had more than double the risk of painful diabetic neuropathy and significantly elevated inflammatory markers (IL-6 and TNF-alpha) in their nerve tissue.
A randomized, placebo-controlled trial of intramuscular vitamin D supplementation in Egyptian prediabetic patients with neuropathy (published in BMC Endocrine Disorders, 2022) found that correcting vitamin D deficiency significantly improved neuropathic pain scores and balance test results compared to placebo.
Dosage used in studies: Get your 25-hydroxyvitamin D levels tested first. Aim for blood levels between 40-60 ng/mL. Most adults over 60 need 2,000-4,000 IU of vitamin D3 daily to maintain adequate levels, according to the Endocrine Society. Your doctor may prescribe higher doses short-term if you’re severely deficient.
Safety notes: Vitamin D is fat-soluble, so it can accumulate. Don’t exceed 4,000 IU/day without medical supervision. High doses over time can cause hypercalcemia (excess calcium in the blood), leading to kidney stones and other problems.
Blood sugar control is critical for preventing diabetic neuropathy progression. Our evidence-based guide to natural blood sugar support covers ingredients that may help keep glucose in a healthy range.
6. Magnesium: NMDA Receptor Support for Nerve Pain
Magnesium plays a direct role in nerve signaling by blocking NMDA receptors, which are involved in pain sensitization. When magnesium levels are low, these receptors become overactive, amplifying pain signals from damaged peripheral nerves. A 2025 review published in Nutrition Research examined the evidence linking magnesium to diabetic neuropathy and found that oral magnesium supplementation helped restore magnesium levels and provided measurable clinical benefits in diabetic neuropathy patients.
The challenge with magnesium research is that most neuropathy-specific studies have used intravenous administration. A study in the Journal of Pain and Symptom Management found that IV magnesium sulfate (500 mg to 1 g) significantly improved pain intensity scores in cancer patients with neuropathic pain. For postherpetic neuralgia (nerve pain after shingles), IV magnesium reduced pain scores significantly within 20-30 minutes compared to placebo.
Oral magnesium supplementation for neuropathy has less direct trial data, but given that an estimated 50% of Americans don’t meet the recommended daily intake for magnesium (according to USDA dietary surveys), correcting a deficiency is a reasonable first step. Magnesium also supports healthy blood sugar metabolism, which matters for diabetic neuropathy prevention.
Dosage used in studies: 400-600 mg/day of magnesium glycinate or magnesium threonate (better absorbed forms). Magnesium oxide, though cheaper, has poor bioavailability (around 4%).
Safety notes: High doses of oral magnesium can cause diarrhea. People with kidney disease should avoid magnesium supplements unless directed by a doctor, as impaired kidneys can’t clear excess magnesium effectively. Magnesium can also interfere with certain antibiotics and bisphosphonate medications.
7. Curcumin: Anti-Inflammatory Support (Emerging Evidence)
Curcumin, the active compound in turmeric, has shown promise for neuropathic pain in preclinical research, though human data is still limited. A 2021 review in Antioxidants (MDPI) noted that curcumin reduces neuropathic pain in animal models by lowering oxidative stress, suppressing inflammatory cytokines, and inhibiting spinal cord pain signaling pathways.
On the clinical side, a 2025 randomized, double-blind trial published in BMC Cancer tested curcumin in pediatric leukemia patients receiving vincristine (a chemotherapy drug that commonly causes peripheral neuropathy). Patients who received curcumin at 3 mg/kg twice daily for three months had reduced neuropathy severity compared to the control group, with over 94% completing treatment without serious side effects.
The main obstacle with curcumin is bioavailability. Standard turmeric powder delivers very little curcumin to your bloodstream. Formulations that use piperine (black pepper extract), liposomal delivery, or phytosome technology can increase absorption by 20 to 30 times. If you’re going to try curcumin for nerve pain, the formulation matters more than the dose on the label.
Dosage used in studies: 500-1,000 mg/day of a bioavailability-enhanced curcumin formulation. Standard curcumin powder at these doses won’t deliver enough active compound to make a difference.
Safety notes: Curcumin can thin the blood and should be used with caution alongside anticoagulants. It may also lower blood sugar, so monitor glucose if you have diabetes. High doses can cause GI upset in some people.
For a deeper look at turmeric formulations and joint health benefits, check our guide to turmeric supplements for joint pain.
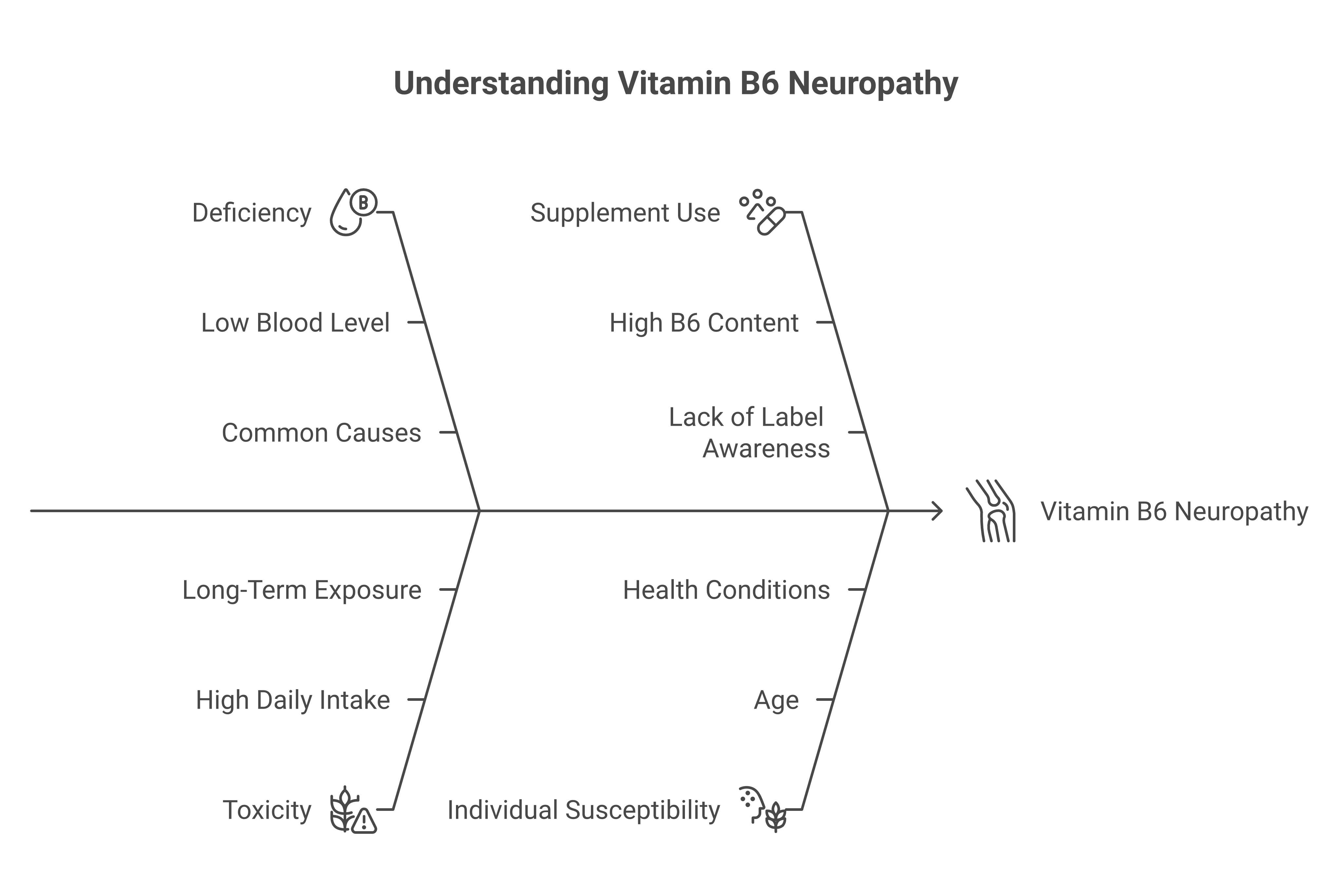
The B6 Warning: When a “Nerve Vitamin” Causes Nerve Damage
This is something most supplement articles don’t mention, and it’s critical. Vitamin B6 (pyridoxine) is often included in nerve health supplements because B6 deficiency can cause neuropathy. But here’s the problem: excess B6 also causes neuropathy, and the toxic dose is lower than many people realize.
According to the NIH’s StatPearls resource on B6 toxicity, sensory neuropathy has been reported at doses as low as 24 mg/day taken over extended periods, though most cases occur above 200 mg/day. The Foundation for Peripheral Neuropathy specifically warns against exceeding 50 mg/day long-term or 2 g/day at any point. The European Food Safety Authority has set its tolerable upper limit at just 12 mg/day for adults.
The mechanism is unusual: excess pyridoxine (the inactive supplemental form) actually competes with pyridoxal-5′-phosphate (PLP, the active form your nerves use), effectively creating a functional B6 deficiency even though blood levels appear high. The symptoms of B6 toxicity, tingling, numbness, and loss of coordination, mimic the exact neuropathy you’re trying to treat.
If you’re taking a nerve health supplement, a multivitamin, and a B-complex, you could easily be getting 100+ mg of B6 daily without realizing it. Add up all your sources. The good news is that B6 neuropathy usually resolves within six months of stopping the excess supplementation, though recovery can be slow.
Safe range: 1.3-1.7 mg/day is the recommended daily allowance. Stay below 50 mg/day from all sources combined unless specifically directed by your doctor.
How to Build a Supplement Stack for Foot Neuropathy
Based on the evidence above, here’s a practical approach. Start with the supplements that have the strongest evidence and address common deficiencies first.
Tier 1 (strongest evidence, start here):
- Alpha-lipoic acid: 600 mg/day on an empty stomach
- Methylcobalamin (B12): 1,000 mcg/day (get levels tested first)
- Vitamin D3: 2,000-4,000 IU/day (get levels tested first)
Tier 2 (good evidence, add if Tier 1 isn’t enough):
- Benfotiamine: 300 mg twice daily (especially for diabetic neuropathy)
- Acetyl-L-carnitine: 1,000 mg three times daily
Tier 3 (supportive, emerging evidence):
- Magnesium glycinate: 400-600 mg/day
- Curcumin (bioavailability-enhanced): 500-1,000 mg/day
Don’t start everything at once. Add one supplement at a time, wait two to four weeks, and track your symptoms. A simple daily journal noting pain levels (0-10 scale), tingling severity, and sleep quality will help you figure out what’s actually working versus what isn’t.
If you’re looking for a formulated nerve support option that combines several of these ingredients, PRO60+ Deep Nerve Renew was designed specifically for adults over 60 dealing with peripheral neuropathy.
What Else Matters Beyond Supplements
Supplements work best as part of a broader strategy. Here are the non-supplement factors that significantly affect neuropathy outcomes:
Blood sugar control: For diabetic neuropathy, maintaining an A1C below 7% is the single most effective way to slow nerve damage progression. No supplement can overcome chronically elevated blood sugar.
Exercise: A 2017 Cochrane review found that regular aerobic exercise improved nerve conduction velocity and reduced neuropathic pain in diabetic patients. Walking 30 minutes daily is a reasonable starting point if your feet allow it.
Alcohol reduction: Alcohol is directly toxic to peripheral nerves and depletes B vitamins. If you drink regularly and have neuropathy, reducing alcohol intake is more important than any supplement you could add.
Medication review: Some medications (statins, certain antibiotics, chemotherapy agents) can cause or worsen peripheral neuropathy. Ask your doctor or pharmacist to review your medication list for neurotoxic drugs.
Healthy skin integrity matters too. Neuropathy in the feet increases the risk of unnoticed injuries and slow healing. Our supplements for aging skin after 60 guide covers nutrients that support skin repair and barrier function.
Collagen supplementation may also support the connective tissue surrounding peripheral nerves. Learn more in our collagen supplement guide for women over 60.
Frequently Asked Questions
What is the best supplement for neuropathy in feet?
Alpha-lipoic acid (ALA) at 600 mg/day has the strongest clinical evidence for reducing neuropathy symptoms in the feet. The ALADIN trial showed a 63.5% reduction in total symptom scores for foot neuropathy. For people with confirmed B12 deficiency, methylcobalamin at 1,000 mcg/day is equally important. Many clinicians recommend both together as a first-line supplement approach.
Can supplements actually repair nerve damage in feet?
Most supplements reduce symptoms (pain, tingling, numbness) rather than reversing structural nerve damage. The exception is acetyl-L-carnitine, which showed evidence of nerve fiber regeneration in sural nerve biopsies at 3,000 mg/day over one year (Sima et al., Diabetes Care, 2005). B12 supplementation can also restore nerve function when the neuropathy was caused by B12 deficiency. Supplements work best when started early, before nerve damage becomes severe.
Is vitamin B6 safe to take for neuropathy?
B6 requires caution. While B6 deficiency causes neuropathy, excess B6 also causes it. Sensory neuropathy has been reported at doses as low as 24 mg/day over extended periods. The European Food Safety Authority recommends no more than 12 mg/day for adults. If you take multiple supplements, add up your total B6 intake from all sources. Stay below 50 mg/day unless your doctor specifically prescribes a higher dose after testing your levels.
How long do neuropathy supplements take to work?
Clinical trials typically show measurable improvements within three to six weeks for alpha-lipoic acid and benfotiamine. B12 supplementation may take three to six months to show full benefits, especially if nerve damage has been progressing for years. Acetyl-L-carnitine trials measured outcomes at 26 and 52 weeks. Track your symptoms weekly and give each supplement at least four to six weeks before judging its effectiveness.
Should I take neuropathy supplements if I have diabetes?
Yes, but with medical supervision. Alpha-lipoic acid and benfotiamine have been studied specifically in diabetic neuropathy populations. Both can affect blood sugar levels, so your diabetes medications may need adjustment. Metformin users should pay special attention to B12 levels, as metformin depletes B12 over time. Always inform your endocrinologist or primary care doctor about any supplements you’re taking.
Are there supplements that make neuropathy worse?
Yes. Excess vitamin B6 (pyridoxine) above 50 mg/day can cause or worsen peripheral neuropathy. Some herbal supplements and weight loss products contain neurotoxic ingredients. High-dose niacin (vitamin B3) can occasionally worsen nerve symptoms. Always check the full ingredient label and total daily intake across all supplements you’re taking.
Can I take neuropathy supplements with prescription nerve pain medications?
Most supplements on this list can be taken alongside gabapentin, pregabalin, or duloxetine, but interactions exist. Alpha-lipoic acid may enhance the blood-sugar-lowering effects of diabetes medications. Acetyl-L-carnitine can interact with blood thinners. Magnesium can reduce absorption of certain antibiotics and bisphosphonates. Consult your pharmacist for a complete interaction check before combining supplements with prescription medications.




